The practice of Hadi Zambarakji
The practice of Hadi Zambarakji

Guide to Acquired Retinoshisis
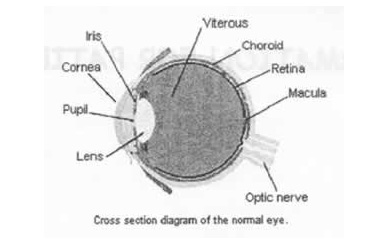
THE RETINA
The retina is the light sensitive layer at the back of the eye (film) which transmits the messages along the optic nerve to the brain. Light rays enter the eye through the transparent (clear) cornea, and must pass through the lens and vitreous (a jelly-like substance) before reaching the retina.
What is acquired retinoschisis?
Aquired retinoshisis (AR) is the result of gradual splitting of the retina into 2 distinct layers. This condition is age related, as it has been reported in patients in the third decade (20-30 years). AR develops from the coalescence of intraretinal microcysts located in the peripheral retina and may extend posteriorly into the central macula where it may affect the vision.
How common is AR?
The prevalence is high in the normal population (4-22% of individuals older than 40 years).
What are the symptoms of AR?
Often, no visual changes occur. AR usually remains stationary over many years. Occasionally AR may progress into the central retina (the macula) and may affect the vision, which is rare. If progression of AR occurs, it is usually slow and would occur over several months or even years, but this varies from patient to patient.
Retinal detachment may occur in a small percentage of patients, as a result of the development of a break in the retina leading to a defect in the peripheral visual field and/or decreased visual acuity. The development of a retinal detachment would need surgical treatment.
What should I do?
You should immediately report any acute change in your symptoms. Specifically, you should report to your Ophthalmologist if you develop a visual field defect (a black curtain coming into your field of vision), any flashes of flight or floaters.
Note:
AR should not be confused with congenital retinoshisis.
Prepared by Mr. H.J. Zambarakji FRCOphth, D.M
Consultant Ophthalmic surgeon
Search the RetinaCare website
Visual guides
 Vitreomacular traction and small macular hole successfully treated with intravitreal Ocriplasmin
Vitreomacular traction and small macular hole successfully treated with intravitreal Ocriplasmin
 Macular hole (pre and post op)
Macular hole (pre and post op)
 Epiretinal membrane (pre and post op)
Epiretinal membrane (pre and post op)
 Diabetic retinopathy (medical management and laser photocoagulation)
Diabetic retinopathy (medical management and laser photocoagulation)
 Traction diabetic retinal detachment (pre and post op)
Traction diabetic retinal detachment (pre and post op)
READ HADI’S LATEST NEWS