The practice of Hadi Zambarakji
The practice of Hadi Zambarakji

Guide to Diabetic Retinopathy
Diabetes Can Affect Sight
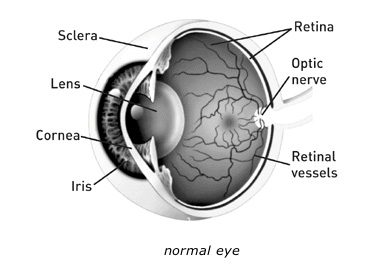
If you have diabetes mellitus, your body does not use and store sugar properly. High blood-sugar levels can damage blood vessels in the retina, the nerve layer at the back of the eye that senses light and helps to send images to the brain. The damage to retinal vessels is referred to as diabetic retinopathy.
Types of Diabetic Retinopathy
There are two types of diabetic retinopathy: Background diabetic retinopathy (BDR) and proliferative diabetic retinopathy (PDR).
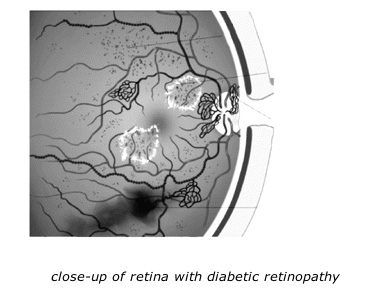
Background retinopathy, is an early stage of diabetic retinopathy. In this stage, tiny blood vessels within the retina leak blood or fluid. The leaking fluid causes the retina to swell or to form deposits called exudates.
Many people with diabetes have mild BDR, which usually does not affect their vision. When vision is affected it is the result of macular oedema and/or macular ischemia.
- Macular oedema is swelling or thickening of the macula, a small area in the center of the retina that allows us to see fine details clearly. The swelling is caused by fluid leaking from retinal blood vessels. It is the most common cause of visual loss in diabetes. Vision loss may be mild to severe, but even in the worst cases, peripheral vision continues to function.
- Macular ischemia occurs when small blood vessels (capillaries) close. Vision blurs because the macula no longer receives sufficient blood supply to work properly.
PDR is present when abnormal new vessels (neovascularization) begin growing on the surface of the retina or optic nerve. The main cause of PDR is widespread closure of retinal blood vessels, preventing adequate blood flow. The retina responds by growing new blood vessels in an attempt to supply blood to the area where the original vessels closed.
Unfortunately, the new, abnormal blood vessels do not resupply the retina with normal blood flow. The new vessels are often accompanied by scar tissue that may cause wrinkling or detachment of the retina.
PDR may cause more severe vision loss than BDR because it can affect both central and peripheral vision.
Proliferative diabetic retinopathy causes visual loss in the following ways:
Vitreous haemorrhage: The fragile new vessels may bleed into the vitreous, a clear, gel-like substance that fills the center of the eye. If the vitreous haemorrhage is small, a person might see only a few new dark floaters. A very large haemorrhage might block out all vision.
It may take days, months, or even years to resorb the blood, depending on the amount of blood present. If the eye does not clear the vitreous blood adequately within a reasonable time, vitrectomy surgery may be recommended.
Vitreous haemorrhage alone does not cause permanent vision loss. When the blood clears, vision may return to its former level unless the macula is damaged.
Traction retinal detachment: When PDR is present, scar tissue associated with neovascularization can shrink, wrinkling and pulling the retina from its normal position. Macular wrinkling can cause visual distortion. More severe vision loss can occur if the macula or large areas of the retina are detached.
Neovascular glaucoma: Occasionally, extensive retinal vessel closure will cause new, abnormal blood vessels to grow on the iris (colored part of the eye) and block the normal flow of fluid out of the eye. Pressure in the eye builds up, resulting in neovascular glaucoma, a severe eye disease that causes damage to the optic nerve.
How is diabetic retinopathy diagnosed?
A medical eye examination is the only way to detect changes inside your eye.
If your ophthalmologist finds diabetic retinopathy, he or she may order color photographs of the retina, Optical Coherence Tomography (OCT) scans of the retina or a special test called fluorescein angiography to find out if you need treatment. In this test a dye is injected into your arm and photos of your eye are taken to detect where fluid is leaking. The OCT scan does not involve any injections and gives the Ophthalmologist additional information about retinal leakage and is very helpful for assessing and monitoring diabetic macular oedema.
Vision loss is largely preventable
If you have diabetes, it is important to know that today, with improved methods of diagnosis and treatment, only a small percentage of people who develop retinopathy have serious vision problems. Early detection of diabetic retinopathy is the best protection against loss of vision.
You can significantly lower your risk of vision loss by maintaining strict control of your blood sugar and visiting your ophthalmologist regularly.
How is diabetic retinopathy treated?
The best treatment is to prevent the development of retinopathy as much as possible. Strict control of your blood sugar will significantly reduce the long-term risk of vision loss from diabetic retinopathy. If high blood pressure and kidney problems are present, they need to be treated. Other important measures include optimizing your cholesterol, taking a healthy diet and avoiding smoking.
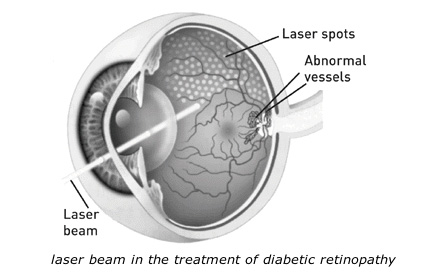
Laser: Laser is often recommended for people with macular oedema, PDR, and neovascular glaucoma.
For macular oedema, the laser is focused on the damaged retina near the macula to decrease the fluid leakage. The main goal of treatment is to prevent further loss of vision. It is uncommon for people who have blurred vision from macular oedema to recover normal vision, although some may experience partial improvement. A few people may see the laser spots near the center of their vision following treatment. The spots usually fade with time but may not disappear.
For PDR, the laser is focused on all parts of the retina except the macula. This panretinal photocoagulation treatment causes abnormal new vessels to shrink and often prevents them from growing in the future. It also decreases the chance that vitreous bleeding or retinal distortion will occur.
Multiple laser treatments over time are sometimes necessary. Laser surgery does not cure diabetic retinopathy and does not always prevent further loss of vision.
Laser for neovascular glaucoma would reduce the risk of total loss of vision and would reduce the risk of developing a painful eye. There are several types of lasers that can be used for this purpose depending on the stage of neovascular glaucoma. In the very advanced stages, laser is performed to reduce the intraocular pressure by ablating the ciliary processes where acqueous fluid production takes place. In some instances, an injection of an anti-VEGF agent may be needed to control the intraocular pressure in patients with neovascular glaucoma.
Anti-VEGF treatments
VEGF stands for “vascular endothelial growth factor”. Several studies have demonstrated elevated levels of VEGF in the vitreous cavity in patients with PDR and macular oedema. These studies have also demonstrated that treatment with anti-VEGF can reduce vascular leakage and improve vision secondary to macular oedema. There are 3 anti-VEGF agents in use for diabetic macular oedema, these are Bevacizumab (Avastin) Ranibizumab (Lucentis) and Aflibercept (Eylea). Lucentis and Eylea are the only anti-VEGF drugs that are currently licensed for the treatment of diabetic macular oedema, but all 3 agents have been used extensively for this purpose. We do not have extensive data comparing visual outcomes in diabetic macular oedema with Avastin, Lucentis and Eylea, but preliminary data suggests that all 3 are effective and relatively safe. On average, when visual acuity loss is mild, all 3 agents appear similar, however, when visual acuity loss is more severe, Eylea is more effective at improving vision. There is however data for the treatment of neovascular macular degeneration, where visual outcomes were similar when comparing Avastin and Lucentis, although subtle differences in outcomes have been noted (see macular degeneration handout).
Other treatments for diabetic macular oedema: Intraocular steroid injections with Triamcinolone used to form an important part of the management of diabetic macular oedema in patients who had persistent macular oedema despite laser treatment. Triamcinolone has now fallen out of favour because of the secondary elevated intraocular pressure and the significantly increased chance of developing cataract. Novel steroids including a dexamethasone implant called Ozurdex and another long acting Fluocinolone steroid implant called Iluvien have received marketting authorization for the management of chronic diabetic macular oedema. Ozurdex also has marketting authorisation in macular oedema secondary to retinal vein occlusion, and can be effective for up to 6 months. Iluvien, which can be effective for up to 3 years has marketing authorization for the treatment of diabetic macular oedema in the EU. The response observed with Ozurdex in retinal vein occlusion is very encouraging (see Retinal vein occlusion handout).
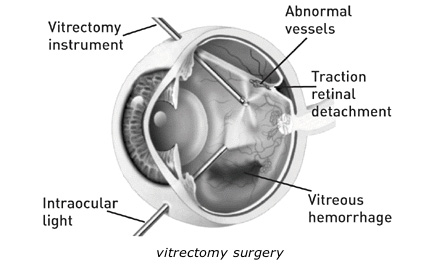
Vitrectomy: In advanced PDR, the ophthalmologist may recommend a vitrectomy. During this microsurgical procedure, which is performed in the operating room, the blood-filled vitreous is removed and replaced with a clear solution. The ophthalmologist may wait for several months to see if the blood clears on its own before performing a vitrectomy.
Vitrectomy often prevents further bleeding by removing the abnormal vessels that caused the bleeding. If the retina is detached, it can be repaired during the vitrectomy surgery. Surgery should usually be done early because macular distortion or traction retinal detachment will cause permanent visual loss. The longer the macula is distorted or out of place, the more serious the vision loss will be.
Prepared by Mr. H.J. Zambarakji FRCOphth, D.M
Consultant Ophthalmic surgeon
Search the RetinaCare website
Visual guides
 Vitreomacular traction and small macular hole successfully treated with intravitreal Ocriplasmin
Vitreomacular traction and small macular hole successfully treated with intravitreal Ocriplasmin
 Macular hole (pre and post op)
Macular hole (pre and post op)
 Epiretinal membrane (pre and post op)
Epiretinal membrane (pre and post op)
 Diabetic retinopathy (medical management and laser photocoagulation)
Diabetic retinopathy (medical management and laser photocoagulation)
 Traction diabetic retinal detachment (pre and post op)
Traction diabetic retinal detachment (pre and post op)
READ HADI’S LATEST NEWS